How the growth of outpatient clinics (now the primary patient location for diagnosis and treatment), integrated care models, and changing modes of treatment call for a new look at how to design ambulatory care facilities. Herman Miller Healthcare highlights solutions for creating adaptive and flexible ambulatory care facilities.
What We Know
Consider these facts:
- Between 2010 and 2020, the demand for inpatient services will decrease by 2 percent, while demand for outpatient services will significantly increase by 30 percent.1
- Experts predict a 21 percent increase in outpatient demand over the next 10 years, including procedures, office visits, imaging and physical therapy.2
- Minimally invasive techniques are replacing complex, inpatient procedures with patient treatment.3
These trends underscore the high-growth, high-change nature of ambulatory care facilities—now and into the future as they continue to serve more people in more ways. One example of such change is the multispecialty clinic. In this scenario, services are rotated with a number of practices sharing one facility. This arrangement can be cost-effective for the healthcare practices and diagnostic groups working within the clinic. It can also be more convenient for patients. This model provides an integrated care approach when compared with a single facility occupied by one practice, specialty, or diagnostic group.
A research paper published by Herman Miller in 2010 ("Coordinating Care in an Age of Chronic Illness") explored issues related to the alarming growth of Americans living with chronic conditions. The paper explored the shortcomings of the current healthcare system to successfully and cost-efficiently treat and manage chronic illness. A coordinated healthcare delivery model, as opposed to a siloed one, is necessary to better address the care of those with chronic diseases.4
A key ingredient in a coordinated care model is the location in which care is delivered and patient health is managed. Outpatient clinics will be the number one diagnosis and treatment location for Americans.
The nature of ambulatory care facilities makes them unique. Designing their interiors requires different thinking and planning from designing an acute care facility. Especially as activities within the outpatient clinic evolve, new design approaches are necessary.
Bill Rostenberg, of Anshen+Allen/Stantec Architecture, presented design ideas for ambulatory clinics at the 2010 annual conference of the Health Facility Institute. He notes differences between ambulatory clinics and acute care facilities—and new ways of thinking about outpatient clinics.5
Outpatient facilities are becoming:
- extensions of the Internet
- extensions of home
- places for advanced medicine
- hubs for integrated care teams
- centers of healthcare delivery
- primary points of patient contact
- places where one goes for treatment unless they absolutely require hospitalization or other care locations
- integral component to healthcare affordability and sustainability
- the wave of the future
Rostenberg’s descriptions make clear that the design of an outpatient clinic needs to account for a good deal of change in services and care models, from in-home monitoring to group appointments. The integration of technology, which supports digital communication and tools throughout a facility, is one example of the kind of change that is happening now.
A Herman Miller Healthcare researcher visited ambulatory care centers, interviewing staff and observing how facilities and their design functioned. In a handful of clinic visits, the researcher observed a number of things that had changed from the clinic’s initial design and use plan.
- A specialist’s office was moved into an Ob/Gyn office, and the specialist’s former office was rented. A pediatrician’s office was moved elsewhere in the building.
- One office became a stress-test room.
- Since it opened 12 years ago, 12 different physician practices have moved in and out of one clinic.
- Occupational health services moved into the urgent care area; the former occupational health space was rented to house sub-specialties.
The researcher also noted examples of underused areas:
- Colonoscopy and sigmoidoscopy rooms were empty because these procedures were no longer performed at the clinic.
- Physician campsite/drop-in spaces were not used, but hadn’t been reconfigured for another use.
- A consultation room had a PACS-capable computer within it, but the space was rented to a podiatrist, and the technology left unused. The podiatrist used the consult room for triage, enlisting two procedure carts that were wheeled into exam rooms for treatment.
- Physicians decided what and where supplies were stored in each exam room, making it time-consuming for other staff to locate supplies and carry out functions working from room to room.
Our Herman Miller researcher’s observations of a handful of ambulatory care facilities are certainly representative of thousands of clinics throughout the country: Designing and furnishing a clinic only to initial plans and expectations means that the facility will quickly become obsolete. Things will change.
Design Problem
A flexible interior design that can integrate levels of care, types of treatments, and family/patient hospitality—a continuum of care services—offers choices as care processes and approaches shift.
As outpatient facilities become the primary point of patient contact and as healthcare delivery models move toward a holistic and integrated treatment approach, the outpatient facility in which care is delivered needs to be as responsive to change. Outpatient facilities need an adaptive design because they will change, often within their first years of operation.
Design Solution
But what exactly is adaptive design? Think of an outpatient facility as a shell. The exterior walls, windows, roof, and doors create the protective outer shell. But everything within that shell can be flexible and movable. Designing an outpatient clinic to be proactive, rather than reactive, is adaptive design.
The clinic layout we are most familiar with features a lobby and reception area in the front of the building, rows of exam rooms in the center, and physician/staff offices and work areas in the back and along the perimeter. These spaces are most often separated with architectural walls. Utilities, such as plumbing, are assigned to specific rooms and not to others. This design supports a linear approach to care, a model long unchanged.
The facility that supports an integrated continuum of care model will look and act quite differently from the more traditional ambulatory care interior layout.
Dividing a Clinic’s Interior
Dividing a clinic’s interior using moveable wall products creates a flexible method for assigning space and functions. An area divided into eight exam rooms, for example, could become a space with four exam rooms and a diagnostic area.
Full-height moveable walls offer nearly unlimited choices in a facility’s layout. They adapt as providers, procedures, and specialties change. And they offer privacy and structural support. Demountable walls are cost effective, an estimated 60 percent savings over drywall (cost comparison of eight years with 15 percent annual change rates).6
A Herman Miller Healthcare customer in the Midwest outfitted its new cancer clinic with wood-grain laminate demountable walls. The result, says Herman Miller Healthcare designer Kristin Cutshall, is a “beautiful and warm environment for patients and their guests. Our client wanted a residential feel and a beautiful look—more like an art gallery than a clinic. And they wanted their patients to feel pampered.” The clinic includes spa and massage areas. But the beautiful is also practical: The layout of this clinic could be altered with limited downtime and no demolition.
Lobby and Waiting Areas
A common approach to check-in and registration places the lobby and admitting spaces at the main entrance to the clinic. But clinics are beginning to employ new check-in and registration processes. One approach is a self-serve kiosk, where patients verify their information and register. Another is point-of-care check-in and registration process. In this model, a patient is greeted in the waiting area by a staff member or nurse, who ushers the patient to a triage, exam, or treatment room. There the staff member registers the patient and continues with a check of the patient’s vitals. Diagnostic tests may occur, followed by the doctor conducting the treatment or procedure—all within the same room.
A point-of-care model also allows the various practices that occupy the clinic space to share a common lobby area but control the services and experience of their individual practice/patient relationships.

Herman Miller Healthcare and Nemschoff Solution: Soft seating and tables and Herman Miller systems create lobby and waiting areas that offer divided private spaces and small clusters of chairs and sofas.
When check-in and registration is moved to the point-of-care area or assigned to a self-serve kiosk, a waiting area can be designed more specifically for families and friends. Spaces with groupings of seats and divided privacy spaces create a warmer lobby area, quite different from a large open space filled with banks of seats and tables. The Nemschoff portfolio includes lounge and multiple seating options, as well as tables and guest seating within exam rooms. The size and design approach of the lobby and waiting space is easily matched with furniture options of varying scale, style, and choice of healthcare textiles. Space divisions can be created with systems products, such as Resolve or Canvas Office Landscape.
Point-of-care registration is one example of the kind of change that makes the case for flexible interior design. Other changes in patient and staff flow will certainly occur in the future.
Triage and Consulstation Areas
A general care clinic needs to consider triage and consultation spaces. Like point-of-care registration where patient flow is expedited, a similar model can be applied to the process for moving patients through assessment and on to diagnostic tests and treatment without requiring them to move in and out of multiple rooms. A space for taking a patient’s weight and vitals en route to a triage or exam room also streamlines the patient path. Consultation spaces can be located close to treatment spaces and waiting areas, so that the flow of staff and patients is efficient.
Locating a staff work area, storage space, and small meeting area in proximity to triage and exam rooms keeps the patient in place while allowing staff to move easily from records and consulting areas to locating supplies and equipment. Less travel time for staff equals more time with a patient, and less moving around for the patient equals less time waiting and enhanced safety.
An efficient layout promotes better use of time, less waste moving from one location to another, and less square footage required for circulation. If the design enables caregivers to work more efficiently by reducing travel distances and the time spent "hunting and gathering," then they will have more time to spend in direct patient care activities and be more effective in whatever tasks they are performing.
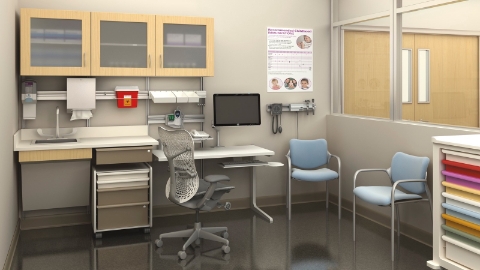
Herman Miller Healthcare Solution: Casework and Co/Struc system, adjustable work surface, and task and guest seating offer a space for diagnosis and discussion. A triage room created with the Compass system and demountable walls can offer greater levels of flexibility, depending on a clinic’s anticipated rates of change.
Patient Care Areas
Ambulatory facilities are often shared by multiple practitioners and practices. A flexible design can fluidly accommodate volume variation in practices, providers, and patients.
Standardized exam rooms promote greater efficiency to the overall facility and use of space. Such an approach provides the necessary furnishings and equipment to all staff members and avoids assigning specific rooms to specific functions. Specialty equipment can be kept in nearby storage areas and then moved into the space as needed.
An adaptive design approach to exam rooms promotes scheduling flexibility and opportunities for integrating services. Shared clinics and flexible exam spaces consider the experience of the patient as well, who can remain in a single room while seeing multiple specialists.
A suite of patient care rooms within a clinic can be furnished with the same configuration of Compass components. The needs of staff and patients are accommodated in a space-efficient layout. Supplies and equipment can be wheeled into the room via mobile procedure carts and lockers. The Compass system integrates with Co/Struc lockers, if attaching the locker to the Compass rail is desired.
Changes to the layout of the room and to locations of med gases, plumbing, and other building services are done quickly with the Compass system, making it an ideal solution for the high-change nature of clinics.

Herman Miller Healthcare Solution: Compass system creates a functional and space-efficient exam room. Components can be reconfigured or rearranged with minimal downtime and no renovation disruption.
Clinical Staff Workspaces
The clinical support spaces that surround patient care rooms also need to be flexible. Staff work areas located close to patient supplies saves time and space. In surgical outpatient clinics, work areas located close to patients are essential.
Designing well-equipped and highly functional observation areas in post-op and recovery help flow and traffic patterns. Storing medication and supplies in these areas helps the staff stay as productive as possible.
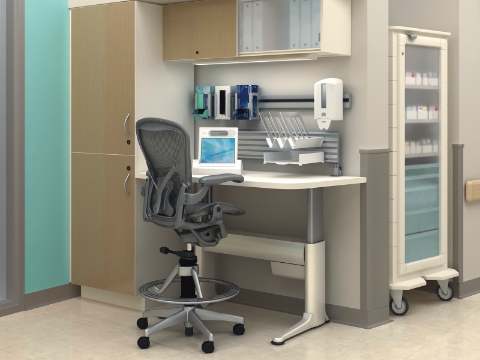
Herman Miller Healthcare Solution: Herman Miller systems, seating, adjustable workstations and surfaces, technology support. Smaller work areas such as this one can be located throughout a clinic, giving staff convenient work spaces.
Staff can also benefit from spaces outside the patient path. A staff module within the clinic may support research, peer consultation, or large group meetings. Ideally, this space can be divided into smaller meeting or work areas as needed.
Designing for a variety of functions in adjacent areas—from medication storage and supplies to linen storage and clinical workspace—reduces a staff’s travel time. It also considers all of the things that a patient needs and places those things close to the patient. Ergonomic considerations, such as lighting, work surface space, and adjustable seating all help staff remain comfortable. “Good lighting is essential to accurately read charts, monitors, equipment, or medication labels,” says Herman Miller Healthcare’s Julie Sless.
In order to provide the communication and regular interaction between healthcare practitioners that a coordinated care model requires, both formal and informal meeting spaces should be considered in a clinic’s design. Says Sless: “Design spaces to facilitate frequent and easy interchange among staff. Collaboration is incredibly important to the quality of the workplace and to sharing experiences and knowledge.”
Clinical Support Spaces
Lab and imaging areas can be located outside of the patient path. In some clinics, lab and radiology groups, like physician practices, are leasing their own spaces from the builder’s owner.
Creating a flexible interior design throughout the clinic ensures that changes and renovations in lab and imaging services can be supported. In addition, a flexible diagnostic work area ensures that subsequent occupants have a space that can be reconfigured cost effectively.
Flexible spaces for lab and imaging services provide function for the present that can be reconfigured with minimal disruption for the future. Mobile workstations and carts are well suited to high-change environments. Furnishings that are flexible and moveable can also be used in other areas throughout the clinic.

Herman Miller Healthcare Solution: Height-adjustable table and Aeron stool, cart and locker, Casework, and technology support create a radiology room. Co/Struc storage provides a good deal of storage capacity without a large footprint.
Planning For The New Now and For What Comes Next
We have been discussing the design of the more traditional functions and spaces in a clinic. But what about some of the other uses and functions within outpatient clinics?
In light of new approaches to treating chronic conditions, as mentioned earlier in this paper, many clinics are rethinking their approaches to care and are including preventative services spaces in their facilities.
Designing an adaptive facility for serving patients with chronic conditions is an important part of a part of a coordinated care approach. Take, for example, a clinic specializing in diabetes care. This facility might integrate a number of functions and activities, creating a diverse and flexible environment for staff and patients. It might offer a dialysis unit and other clinical care spaces. But it might also include a nutrition and kitchen facility for educating on diet and cooking. It might include an exercise room. Beyond physician and nurses, the facility might house pharmacists who assist with medication monitoring and tracking. This same facility may evolve to include new services and new approaches to treatment.
Larger spaces for group appointments are finding their way into outpatient care facilities. An emphasis on community activities is informing the design of Cleveland Clinic’s Community Health Center. Spaces currently used for staff training in acute care facilities may evolve to incorporate patient activities and community events.7 A flexible system for dividing the space further maximizes the multiuse potential.
As the population ages and technology advances, creating greater virtual connections from patients’ homes to a physician or nurse housed in the clinic will become a common form of care. Often referred to as telehealth and e-medicine, these new options are offering benefits such as keeping patients at home and decreasing readmissions and costs of care.
Telehealth spaces accommodate virtual interaction between patients and clinical staff. A pair or pod of workstations can provide the technology and individual space for staff to conduct virtual, one-on-one check-ups with patients.
Adaptive Solutions For Changing Environments
As outpatient clinics outpace acute care facilities as the primary location for patient care, increased attention to the design of the outpatient facility becomes paramount. As the treatments and procedures delivered at ambulatory care facilities expand, so do their impact on the design of the clinic.
A flexible interior design that can integrate levels of care, types of treatments, rehabilitative care, and family/patient hospitality—a continuum of care services—offers choices as care processes and approaches shift. Recall Bill Rostenberg’s earlier descriptions of outpatient facilities, from an extension of the Internet to a center of healthcare delivery.
And recall our Herman Miller Healthcare researcher’s notes on the difficulty of clinic layouts and furnishings to keep pace with changing occupants, changing specialties, and changing services.
A flexible approach to design and furnishings can help a clinic adapt to change. The ideas on product and application solutions presented here are only some of Herman Miller Healthcare’s ideas for designing flexible, expandable outpatient clinics.
Notes
1. sg2, sg2’s 2010 Annual Business and Technology Forecast (member access), "http://www.sg2.com/"sg2.com
2. Johannessen, W., PhD., “Orthopedics Boom: Growth Opportunities in the Decade Ahead,” sg2 Expert Insight, October 4, 2010.
3. Healthcare Financial Management Association, “Ambulatory Care Stands Out Under Reform,” May 1, 2010.
4. Herman Miller Healthcare, "/research/research-summaries/coordinating-care-in-an-age-of-chronic-illness.html" “Coordinating Care in an Age of Chronic Illness,” 2010.
5. Rostenberg, B., FAIA, FACHA, ACHE, EDAC, “ The Ambulatory Care Exemplar: Medicine Beyond the Hospital,” Health Facility Institute Annual Conference, October 25, 2010
6. "http://www.trainormodularwalls.com/inner.php?cid=48" www.trainormodularwalls.com, accessed 4/11/2011.
7. Commins, J., “Cleveland Clinic’s New Health Center Will Feature ‘Patient Navigators’ to Coordinate Care,” Health Leaders Media, June 3, 2010, accessed June 2010.
