The U.S. has the most expensive healthcare system in the world, yet “experts agree that it is riddled with inefficiencies, excessive administrative expenses, inflated prices, poor management, and inappropriate care, waste, and fraud.”1
Clearly, no miracle cure will fix the mess. But perhaps some solutions are hidden in plain sight within organizations that have successfully cut waste, streamlined processes, and become more competitive and prosperous by integrating lean management systems.
What We Know
Almost 15 million patients fall victim to medical error or infections acquired in-hospital every year.2 Of those, 98,000 die from the mistakes, and perhaps as many die from the infections.3
This isn’t because healthcare workers are inept or uncaring. They, too, are often victims of systemic inefficiencies and of complex and ambiguous processes. While some estimates place waste in healthcare between 30 and 40 percent, “the reality of what we’ve observed doing minute-by-minute observation over the last three years is closer to 60 percent,” says Cindy Jimmerson, founder of Lean Healthcare West.4 In fact, when one director of process improvement tracked nurses on a typical shift, he found they typically travel over five miles, much of it in wasted motion.5
American manufacturing has been fighting waste in all its forms for several years. Popular tools for doing so include the Toyota Production System (TPS) and Motorola’s Six Sigma. As a result, American manufacturing, once in decline, is experiencing a remarkable renaissance as a leader on the world stage.
Does healthcare have anything to learn from manufacturing? Might TPS, the lean practice that has been so successful for many companies, apply to healthcare, too?
Absolutely, say those who have experienced life on both sides of the fence, in manufacturing and in healthcare. Furthermore, several pioneering healthcare organizations have adopted lean production systems, and now, several years into the transition, are reaping the same benefits that transformed American manufacturing.
What lean means
The concept of lean manufacturing has trickled into public consciousness as catchphrases about eliminating waste and cutting cost. While that’s part of the picture, TPS is more substantial than buzzwords and more comprehensive than a weekend workshop. It requires an organization-wide commitment to analyzing work processes in order to systematically and continually improve them. Lean requires the participation of every individual in the organization, from the line worker (or the CNA) to the CEO. It isn’t easy to incorporate, and it isn’t a quick fix, but it can be incredibly effective.
The basic approach of TPS is to first understand the needs of the customer, then “go and see” every step of a process, whether it’s admitting a patient to the ER or installing a dashboard in a car, to determine whether it adds value in the customer’s eyes or is waste. Ambiguity is removed from processes by clarifying who is responsible for each task and exactly how and when that task will be performed. As problems are uncovered or better ways to complete the task are identified, they are addressed immediately with quick experiments to test the change. In that way, flexibility is built into fixed processes, and “root problems” are uncovered and corrected before they become embedded in the system.
Ideally, work flows smoothly (rather than in batches) along the simplest, most direct route and is performed the same way every time. Work is “pulled” through the line according to customer demand. And it is evaluated continually to improve the process.
All this is well and good for manufacturing, but how does it apply to healthcare? Caring for sick people isn’t like building a car. Or is it?
Lean for Healthcare
“Without question. The issues and problems are similar and can be addressed with similar processes,” says Steve Palmreuter, performance improvement coordinator, St. Mary’s Healthcare in Grand Rapids, Michigan. After implementing TPS at Herman Miller for many years, Palmreuter sought to bring those same processes to a major healthcare system in his local community. “The potential I see here for healthcare is tremendous,” he says.
According to Dr. Steven Spear, professor at Harvard Business School, the problem in healthcare arises when extremely complex processes are swathed in ambiguity about who is responsible for what tasks and exactly when and how they should be performed. Thus, opportunity for error is high, and there is no systematic way to address problems. “As a result, people confront ‘the same problem, every day, for years’ (as one nurse framed it for me) regularly manifested as inefficiencies and irritations—and, occasionally, as catastrophes.”6 As in other industries, employees become adept at working around problems rather than at solving them.
It doesn’t have to be this way. The stories emerging from healthcare organizations that have adopted lean practices point to striking improvements in patient care, elimination of waste and inefficiency, and the associated impact on cost. For example, central-line catheters that are placed in veins leading to the heart may speed the delivery of medication, but they can be deadly places for infection. Nationally, 250,000 patients contract central-line-associated bloodstream (CLAB) infections every year, and 15 percent of them die.7
At LifeCare hospital in Pennsylvania, the mortality rate for CLAB infections was 40 percent with cost per infection running between $25,000 and $80,000. By applying lean practices—removing ambiguity, quickly responding to problems, and testing process improvements, such as changing the disinfectant used—LifeCare reduced CLAB infections by 87 percent despite a 9.75 percent increase in lines placed. Other early adopters of lean healthcare practices, such as ThedaCare, Inc., in Appleton, Wisconsin, and the Virginia Mason Medical Center in Seattle, Washington, report similar improvements in patient care as well as annual savings in the millions of dollars.
Park Nicollet Health Services, a major medical center near Minneapolis, Minnesota, for example, reported saving nearly $7.5 million following its first year of top-down implementation of TPS—savings it passed along in lower fees for uninsured patients.8 Metrics like these require a commitment to change—both systemic cultural change as well as ongoing continual rapid experiments to test and improve processes.
While healthcare professionals are well-versed in experimentation and the scientific method, too often that training goes untapped in the top-down culture of healthcare organizations. “Nurses all have scientific degrees, so the concept of problem-solving ought to be familiar,” says Palmreuter, “but the culture interferes with problem solving. That’s a big challenge.”
“If you can get all of your people engaged all the time in making incremental improvements by using basic common sense tools, that’s very powerful,” says Ron Wince, CEO of Guidon Performance Solutions, a consulting firm that applies tools from industry to service organizations.9
Unfortunately, the crisis facing the healthcare industry is only beginning to play out. As the Baby Boom generation begins to stress the system beyond what it has ever absorbed, time to address serious systemic problems is growing short. “Making healthcare affordable today is difficult, but it will only be more challenging when America’s 78 million baby boomers start reaching retirement age in 2010 and place enormous demands on our healthcare system.” says David Wessner, CEO, Park Nicollet Health System.10 Lean isn’t the only solution, but it represents one solid and tested way to streamline processes, identify inefficiencies, reduce costs, and address systemic problems.
Problem Statement
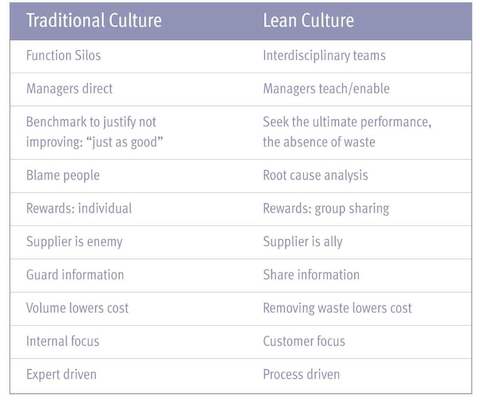
Although factories are different from hospitals, TPS offers the same potential to reduce waste, error, and unnecessary mortalities, to lower costs, to improve employee morale and retention, and to improve patient care. Realizing this potential presents at least two challenges. One is physical: How do you get the best alignment between the facility and the work people do there? The other is cultural: How do you get doctors, nurses, technicians, and everyone else involved to look at what they do in a new way?
Solutions
Herman Miller, Inc., has experience with both challenges. Take the cultural aspect. It was an underperforming subsidiary that first led us to a meeting with Mr. Hajime Ohba, president of Toyota Supplier Support Center (TSSC), over 12 years ago. Soon after Mr. Ohba’s visit, we became one of only 200 companies in the U.S.—and the only office furniture manufacturer—chosen to participate in a special mentoring relationship with TSSC.
In the ensuing years, the problem subsidiary became Herman Miller’s best performer with the shortest lead-times and the highest margins. From 126 assembly employees running three shifts and struggling to produce 6,000 pedestal files a week, it now produces 8,000 units weekly with 22 people on two shifts in about half the space it occupied in 1996. “The turnaround of our facility was so significant that it got everyone’s attention,” says Matt Long, corporate director of continuous improvement, Herman Miller.
In 2000, the entire Herman Miller organization adopted the Toyota Production System as its sole management and manufacturing process. Toyota has designated Herman Miller a “showcase” company for TPS, and we regularly host other companies, including major healthcare organizations such as Mayo Clinic, that come to observe lean manufacturing in action.
A design perspective on lean environments
Park Nicollet Health Services, which includes a 426-bed hospital, a 25-location network of clinics, an institute, a foundation, and some 8,200 employees, began implementing TPS in 2004. The initiative is ongoing as every department continues to systematically analyze its processes—charting the paths patients follow, timing how long they wait and the route caregivers follow—in order to eradicate redundancy and waste. The Endoscopy Department, for example, implemented a “waterfall” patient schedule to create a steady flow rather than scheduling patients in 15-minute batches. Lights outside exam rooms indicate when patients are ready to move to the next stage—providing a visual cue to “pull” patients through the system. A more efficient way to restock supplies was designed.

Flexibility and modularity support the changes associated with lean process improvement.
As a result, the department doubled its capacity even while caregivers spent more time with patients. “My work experience is more satisfying because I’m spending more time with my patients and less time chasing things down that should be there,” commented the department chair.
When an organization changes its processes, however, the physical environment also has to change. As the Endoscopy Department determined the most efficient way to track and route patients, walls had to come down and equipment had to be moved around. As it changed the way it stored supplies, the storage containers also had to change.
With lean processes, inventories are small; batch sizes are small; and small experiments to improve processes are run continually. Without the ability to change the environment, an organization has to work around it. Then, “the process adapts to the physical environment rather than the physical environment adapting to the process,” says Renee Hawk, healthcare designer for Herman Miller. When the physical environment is fixed and immovable, it becomes an impediment rather than a support to implementing lean.
Peggy Vogel, healthcare designer for Herman Miller, notes that when Park Nicollet renovates a space, it takes a systematic approach to design. First, the analysis of each department’s processes and flow is thorough and exhaustive, and Vogel is often asked to participate early in order to understand those processes and to help identify solutions. Then, “we actually mock up a procedure room and install product to test the proposed processes,” says Vogel. Rather than focus on cost, aesthetics, or “the way we’ve always done it,” this customer’s priority is to achieve the best function and most flexible solution—qualities that are at the heart of lean.
The advantages of a best-functioning, most-flexible solution was clear when a new lab in a large Florida hospital suddenly lost 3.5 full-time equivalents (FTEs) due to budget cuts. “The lab was completely installed when the new lab manager decided to incorporate lean processes to make up for the loss of staff,” says Nancy Harwell, healthcare designer, Herman Miller.
Since the lab was furnished with Herman Miller modular products and flexible casework, the traditional departments were quickly redesigned into three work cells: automated, semi-automated, and manual. By routing specimens that required similar processes to the same cell (80 percent were processed automatically), the lab was able to handle the same workload with fewer FTEs.
In her report on the design of this laboratory, the manager wrote: “When designing the layout of a lean laboratory, flexibility is of key importance.…Adaptability and expandability within the laboratory can be greatly improved by the investment of flexible casework. Flexible casework provides a convenient method for easily modifying and configuring work cells.”
In clinical applications, lean is simple, functional, and moveable—no unnecessary surfaces, extra storage, or built-in components. Supplies are restocked daily—just-in-time, not just-in-case.
Lean procedure rooms that healthcare designer Peggy Vogel did for Park Nicollet are simply equipped with Co/Struc C frames, countertops, and drawers hanging on wall rails. “They’re modular and flexible to the max,” says Vogel. This approach discourages hoarding supplies and lends itself to quick readjustments as well as to infection control, since components are restocked regularly and can be cleaned easily.
As these examples show, and as Palmreuter and others note, while healthcare differs from manufacturing, the fundamental processes are the same. Based on the testimonials emerging from early adopters of lean principles in healthcare and Herman Miller’s work with healthcare organizations, the results of implementing lean are promising. They include
- Empowered and energized staff
- Improved patient care with markedly fewer medical errors and mortalities
- Increased efficiencies and reduced costs with associated avoidance of costly expansions in facilities and equipment
The option to maintain the status quo is unsustainable. The good news for healthcare is that lean processes have been thoroughly vetted by organizations like Herman Miller for many years.
The better news, however, is that Herman Miller has the products and expertise to help hospitals implement a lean approach. Lean represents real hope for organizations desperately in need of change. Herman Miller can help them apply lean to control costs even as they are improving patient outcomes.
Notes
1.“Health Insurance Cost,” National Coalition on Healthcare, 2008.
2. Sharkey, Michael, “Healing the hospital: The Toyota Production System and healthcare?” Health Executive 3, no. 2 (Feb. 2007).
3. Spear, Steven J., “Fixing Healthcare from the Inside, Today,” Harvard Business Review (Sept. 2005): 1.
4. Quoted in “Lean Healthcare? It Works!” Industry Week, (1 Nov. 2003).
5. Andel, Tom, “Thinking lean: The cure for what ails you.” Logistics Management, 46, no. 8 (1 Aug. 2007).
6. Spear, Fixing Healthcare, 3.
8. Park Nicollet Health Services, “Park Nicollet: National Leader in Applying ‘Lean Production’ to Healthcare,” press release, 23 March 2005.