Lean Lives in Adaptive Settings
Download PDF (2.75 MB)
Key Insights
- Originally developed for manufacturers, lean methodologies can reduce waste in healthcare.
- Because change is inherent to continuous improvement, physical environments that are adaptive support the move to lean.
- Itself a lean organization with a history in adaptive design, Herman Miller is uniquely suited to work with hospitals interested in implementing lean practices.

1. Useless motion
Example: equipment and supplies stored in hard-to-reach places that cause back injury or fatigue
2. Waste from overproduction
Example: ordering unnecessary diagnostic tests or medication
3. Waste and scraps and defects
Example: misdiagnosis or mistakes in surgery
4. Waste from transportation and handling
Example: constantly moving patients and supplies
5. Waste from waiting times
Example: to see the doctor or for test results
6. Excess processing
Example: creating more work than necessary by asking patients to show their insurance cards several times during the same visit
5. Waste related to useless and excess inventories
Example: medications and supplies
As patients continue to develop a consumer mindset, hospitals are under pressure to reduce costs, improve quality, promote safety, and enhance the patient experience in order to stay competitive.
In response, many hospitals are implementing lean practices. The idea of maximizing customer value while minimizing waste—the intent of lean—is especially attractive to hospital administrators; an estimated 30 to 60 percent of hospital costs are related to unnecessary processes and inefficiencies.1 These include everything from information systems that don’t communicate with each other to inefficient floor plates that, at the very least, increase walking distance.
While lean methodologies were originally developed for manufacturers, they work in healthcare environments because the principles behind them are universal. For instance, the Toyota Production System’s seven types of waste in manufacturing are consistent in healthcare settings.2
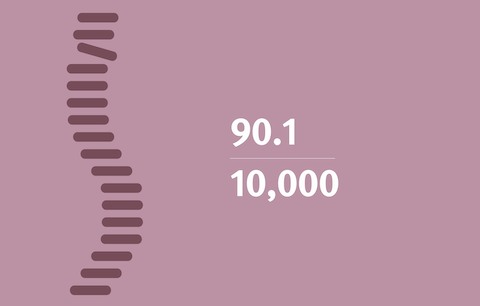
Diagnosing Numbers: Hospital employees miss more work due to back injuries than coal miners. The incidence rate for back injuries involving lost workdays was 90.1 per 10,000 full time workers in US hospitals. The incidence rate for miners was 56.3.3
Room for Improvement
While decreasing waste is an important aspect of lean, a goal of continuous improvement is at its very core. If one were to distill lean philosophies, they would find examples of continuous improvement; such as building value, saving time, creating efficiency, and removing waste, all while promoting safety.
Because changing a process in one part of any system creates a ripple effect, a commitment to lean means an obligation to continuous improvement across the entire enterprise—not just one aspect, sector, or segment. And, not just as an instance, but on an ongoing basis (as the word “continuous” clearly indicates).
Change is inherent to continuous improvement, and that has implications for any setting. For that reason, a lean environment must be adaptive, or intentionally designed to accommodate change. While facility changes alone can’t result in a lean operation, the physical environment can be a tool to support the move, or the journey as Toyota calls it, to lean. Organizations aspiring to change processes, technology, and culture are more successful when they use facility design to support and reinforce those changes.4
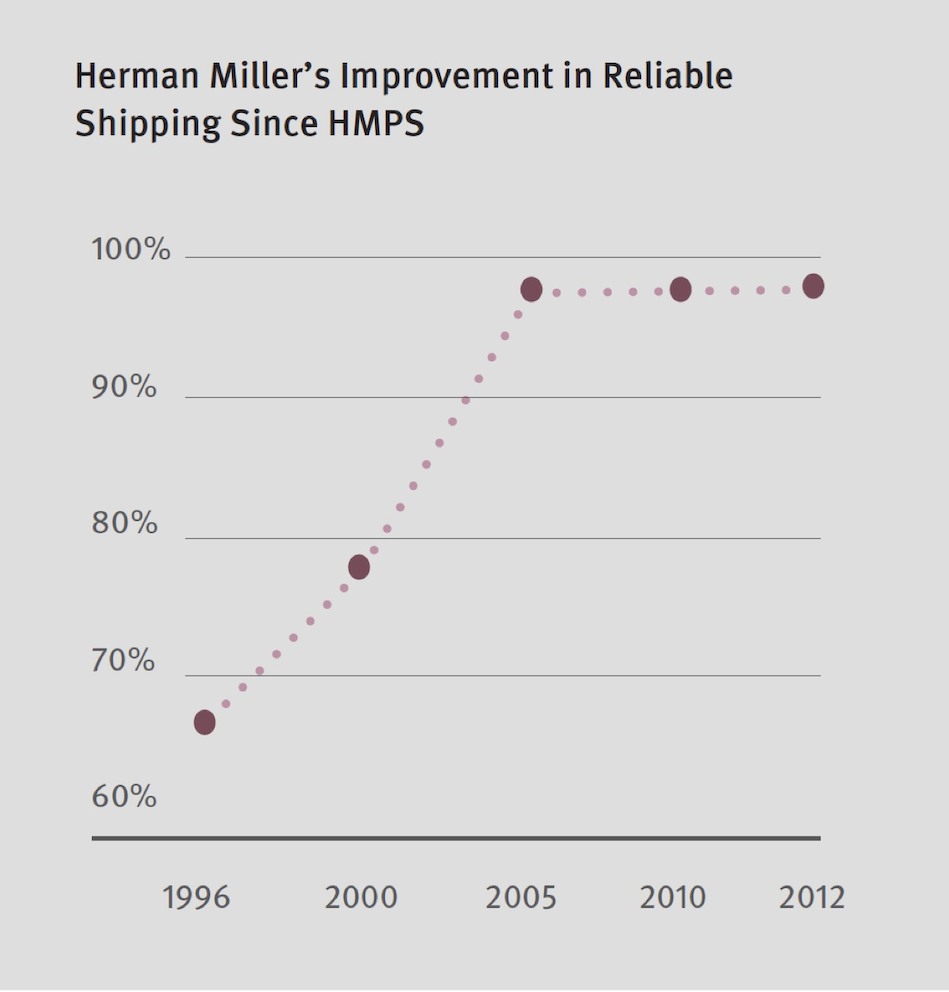
Herman Miller, which implemented a version of the Toyota Production System with great success more than twenty years ago, has extensive experience creating environments that can adapt to continuous change—the very kind of change inherent to lean methodologies. Herman Miller continues to implement the Herman Miller Performance System (HMPS) today, through its exclusive relationship with the Toyota Production System Support Center.
Robert Propst, who was Director of Herman Miller Research in the 1960s, often drew on personal experience for his work: “He was usually dissatisfied with conditions as he experienced them,” wrote Hugh De Pree, Herman Miller’s CEO at the time.5 It was while Propst was a patient at the University Hospital in Ann Arbor, Michigan, that he conceptualized the Co/Struc system, the original moveable modular system for healthcare.6
Propst was frustrated by the inability of both the hospital and the office to handle changes already happening—and the changes that were sure to come. “Human organizations have always been natural places of change, reflecting the organic nature of life,” he wrote. “What is different now is the pace of change and the prospect that it will come faster and faster.”7
In response, he defined nine criteria for adaptive spaces. And just as the rules of lean can be applied with great effect to healthcare, Propst’s criteria can be applied to healthcare environments. In fact, when considered through the lens of continuous improvement, his criteria show just how prescient Propst was about change and its implications for an environment’s flexibility.
As the rate of change has increased, Propst’s criteria have increased in significance. A facility designed and equipped using his criteria will more likely have the ability to keep up with changes that result from process improvements. Or to put it another way, the success of lean initiatives, particularly in healthcare, are directly related to the ability of the staff to optimize the physical environment in response to changes that build value, save time, create efficiency, and remove waste.
Forgiving
An environment that’s forgiving allows people to change their minds, accommodating change without significant costs or delays. Few, if any, pieces are permanently placed.
Adaptiveness is forgiving. Forgiving spaces allow people to feel better about the inherent changes they will face within them. Particularly in healthcare, things can change at any moment, and almost certainly between the time a facility is planned and when it’s occupied. When they do, it’s the adaptive settings that work best and hardest to produce better outcomes. For example, the leaders at Bluewater Health (Ontario) garnered immediate results when they chose to implement forgiving solutions in 80 percent of their facility renovations. By making the transition to reconfigurable solutions as opposed to fixed ones, Bluewater saw significant savings in cost and energy, as well as the ability to change.
Herman Miller, Bluewater Health case study, 2014. Accessed July 14, 2017: https://www.hermanmiller.com/research/case-studies/bluewater-health/

Coherent
When all the elements of an environment are intuitive, work together seamlessly, and integrate with other systems (e.g., electrical and plumbing), an environment is coherent.
Even if a building or facility takes years to complete, coherent solutions within it allow an interior to be changed or maneuvered in minutes. If products are mindful of the structures in which they’re used, they can provide consistently coherent and reconfigurable solutions. This could mean the difference between hours and months when renovating a space for new treatment methods, or even the inability to change at all.

Process forwarding
A process-forward environment makes it easy and intuitive for people to carry out their tasks, e.g., communicating and handling information. It’s healthy and accommodates people with a diverse set of needs.
While caregiver roles and needs change, many providing care use the same tools, settings, and resources. Propst’s Co/Struc design promoted the idea that various caregivers can use and work from its design in a seamless, organized manner. Practitioners can change or manage their specific needs by simply swapping out a drawer or shelf. We know that more than one person will be using our products for more than one reason, so we design them to be more accommodating for all.

Modular limited
Modular limited means an environment has the fewest number of parts serving the greatest number of functions, and those parts and pieces are easy to assemble.
The original modular system for healthcare, Co/Struc, uses sizes that mathematically work and fit together (including 24-, 48-, and 72-inch) components. This helps the design remain modular and flexible over time. In addition, Co/Struc requires fewer components than systems that have “modules” based on three-inch increments. Staff can easily add, remove, or reconfigure components without tools, dust, disruption, or downtime.

Open-ended
Open-ended environments are able to respond to new situations and people’s needs gracefully and without disrupting visual continuity. New products do not make existing components obsolete.
Herman Miller products are designed to work well together, functionally and aesthetically. Even today’s Compass™ casework offers components that are fitted to integrate seamlessly into Co/Struc’s architecture. Holistic thinking, whether about the environment or about the products within it, results in solutions that fit together, work together, and have complementary colors, materials, and finishes.
Readily available
“Components are stable, and easily obtained with guaranteed quality at a predictable cost,” wrote Propst. “Users must get what they need, when they need it, over the long term.”
In 1971, Herman Miller introduced the Co/Struc System as a set of components that could be reconfigured to meet the needs of healthcare professionals in various hospital departments, including labs and pharmacies. The components are durable, reusable, affordable, and easy to configure or reconfigure into spaces and solutions, even today. Co/Struc’s non-obsolescence allows parts made more than four decades ago to cooperate seamlessly with parts made today, and tomorrow as well. This makes replacing or adding parts to the Co/Struc System easy and reliable.
As the rate of change has increased, Propst’s criteria have increased in significance. A facility designed using his criteria will more likely have the ability to keep up with changes that result from process improvements.

Replaceable
Propst’s definition of replaceable includes easy disassembly of components as well as easy upgrading of a facility without disruption of work processes, and without throwing away the initial investment.
Propst and his colleague Jack Kelley designed Co/Struc more than 40 years ago to be “selectively replaceable.8 Nearly a half century later, Herman Miller designs products that can be changed out and changed up, as needs change. Our products’ flexibility minimizes materials and life-cycle costs to deliver lasting value in parts that are quick—and easy—to replace.

Progressively enterable
When a setting allows people to update it at their own pace, it’s progressively enterable. Sometimes experimentation is a part of the process; other times, tweaking is all that’s needed.
Co/Struc welcomes additions and subtractions as needed. For instance, in a lab setting, if more space or storage is needed, pieces can be easily added or subtracted, changed, or swapped accordingly as needs change. This demonstration of lean systems is seen in our other casework offerings such as Compass, which, like Co/Struc welcomes change in a variety of ways using a variety of parts, pieces, and additional products.
Facility renewing
If a product helps convert existing facilities to new uses, and/or bring fresh capabilities to a facility, and if it works in both new and old facilities, then it’s facility renewing.
We design our products with the certainty of change. Twenty years ago, an exam room was only that—an exam room. Today, some communities of people are better served with a space that can easily toggle between two modes of care: examination and consultation.
These additional product criteria support the goals and practice of lean, as they aim to optimize product function across varied settings for a variety of users. Success in becoming a lean organization, a history in adaptive-design, and a comprehensive product offering make Herman Miller uniquely suited to work with hospitals interested in learning more about what it means to continuously improve settings, and the many ways that settings can support a lean healthcare organization.
What we’ve learned from Toyota helped us improve our lean standards, and, at Herman Miller, we aim to help health systems improve theirs and continue toward their vision, or what Toyota (and the entire lean community) call “True North.”
Organizations committed to creating lean environments see the transition as a journey. Throughout the journey, our experience, knowledge, and our own lean practices can keep your organization’s compass at True North—which we believe may be the right direction for the future of healthcare.
Notes
1. Health Care Advisory Board (HCAB), “More Hospitals ‘Go Lean’ to Reduce Costs and Improve Care Delivery,” Finance Watch, September 3, 2005.
2. Maggie Mallard, “7 Wastes of Lean in Healthcare,” accessed November 28, 2016, https://blog.kainexus.com/improvement-disciplines/lean/7-wastes-of-lean-in-healthcare.
3. American Nurses Association, “Handle with Care Fact Sheet,” accessed November, 28, 2016, http://www.nursingworld.org/MainMenuCategories/ANAMarketplace Factsheets-and- Toolkits/FactSheet.html.
4. Ronda G. Hughes, Mike R. Murphy, John Reiling, “Chapter 28: The Impact of Facility Design on Patient Safety” in Patient Safety and Quality: An Evidence-Based Handbook for Nurses, ed. R.G. Hughes (Agency for Healthcare Research and Quality), April, 2008. Accessed November 28, 2016, https://archive.ahrq.gov/ professionals/clinicians-providers/resources/nursing/resources/nurseshdbk/ nurseshdbk.pdf.
5. Hugh De Pree, Business as Unusual: The People and Principles at Herman Miller (Herman Miller, 1986), 98.
6. Ronda G. Hughes, Mike R. Murphy, John Reiling, “Chapter 28: The Impact of Facility Design on Patient Safety” in Patient Safety and Quality: An Evidence-Based Handbook for Nurses, ed. R.G. Hughes (Agency for Healthcare Research and Quality), April, 2008. Accessed November 28, 2016, https://archive.ahrq.gov/ professionals/clinicians-providers/resources/nursing/resources/nurseshdbk/ nurseshdbk.pdf.
7. Robert Propst, The Office: A Facility Based on Change (Elmhurst, IL: The Business Press, 1968), 12.
8. Herman Miller, Co/Struc: A Coherent Structures System for Hospitals, 1967, 14.
To find out more about lean healthcare practices, settings, or solutions contact [email protected].